ESOPHAGUS

DYSPHAGEA
-
-
-
-

EOSINOPHILIC ESOPHAGITIS
Eosinophilic infiltration of the esophageal mucosa.
Symptoms: dysphagia or food impaction in atopic men in their third to fourth decades of life.
Diagnosis: endoscopic findings of mucosal furrowing or raised white specks (thought to represent eosinophilic microabscesses), and confirmed by histologic examination of the esophageal mucosa.
Treatment: disimpaction of a food bolus. Swallowed topical corticosteroids (fluticasone propionate or beclomethasone).
Eosinophilic infiltration of the esophageal mucosa.
Symptoms: dysphagia or food impaction in atopic men in their third to fourth decades of life.
Diagnosis: endoscopic findings of mucosal furrowing or raised white specks (thought to represent eosinophilic microabscesses), and confirmed by histologic examination of the esophageal mucosa.
Treatment: disimpaction of a food bolus. Swallowed topical corticosteroids (fluticasone propionate or beclomethasone).

GASTROESOPHAGEAL REFLUX DISEASE
- Transient relaxation of LES, Hiatal hernia, delayed gastric empty, poor esophageal clearance
- Heartburn, atypical chest pain, Night cough, chronic hoarseness, chronic sore throat, asthma.
- If simple, typical and no alarm symptoms: PPI
-EGD if : alarm symptoms (dysphagia), failure to respond to treatment, long history of symptoms.
- 24h study if atypical GERD (chronic cough with normal EGD, or refractory symptoms with normal EGD)
H. pylori don't cause GERD
TX: PPI, Fundoplication if doesn't tolerate PPI.
- Transient relaxation of LES, Hiatal hernia, delayed gastric empty, poor esophageal clearance
- Heartburn, atypical chest pain, Night cough, chronic hoarseness, chronic sore throat, asthma.
- If simple, typical and no alarm symptoms: PPI
-EGD if : alarm symptoms (dysphagia), failure to respond to treatment, long history of symptoms.
- 24h study if atypical GERD (chronic cough with normal EGD, or refractory symptoms with normal EGD)
H. pylori don't cause GERD
TX: PPI, Fundoplication if doesn't tolerate PPI.

BARRETTS ESOPHAGUS
- Specialized intestinal epithelium
- Associated with adenocarcinoma
- Tx PPI
- Pathology: Goblet cells
- Surveillance: 2 EGD with bp within 1 year
* If no dysplasia repeat in 3 years
* If low grade dysplasia repeat EGD in 6 months if no higher grade dysplasia repeat yearly until no dysplasia on 2 annual bp
* If high grade dysplasia without mucosal irregularities, resection vs q 3months EGD and bp
- Specialized intestinal epithelium
- Associated with adenocarcinoma
- Tx PPI
- Pathology: Goblet cells
- Surveillance: 2 EGD with bp within 1 year
* If no dysplasia repeat in 3 years
* If low grade dysplasia repeat EGD in 6 months if no higher grade dysplasia repeat yearly until no dysplasia on 2 annual bp
* If high grade dysplasia without mucosal irregularities, resection vs q 3months EGD and bp

ESOPHAGEAL CANCER
-Adeno (distal 1/3 esophagus) and squamous (proximal 2/3 esophagus) almost 50% each
- Squamous : risk factor alcohol+tobacco
- Adenocarcinoma related with Barretts and GERD. Increasing in incidence
- Dx: EGD +biopsy. For staging endoscopic u/s and CT abd and pelvis
-TX
*If small and localized resection
*If large or metastasis chemotherapy with 5FU and cisplatin and radiation prior to surgery
-Adeno (distal 1/3 esophagus) and squamous (proximal 2/3 esophagus) almost 50% each
- Squamous : risk factor alcohol+tobacco
- Adenocarcinoma related with Barretts and GERD. Increasing in incidence
- Dx: EGD +biopsy. For staging endoscopic u/s and CT abd and pelvis
-TX
*If small and localized resection
*If large or metastasis chemotherapy with 5FU and cisplatin and radiation prior to surgery

ZENKER DIVERTICULUM
Outpouching of upper esophagus
Foul smelling breath, regurgitates food from several days before.
Touble initiating solid food swallow.
Tx: surgery
Outpouching of upper esophagus
Foul smelling breath, regurgitates food from several days before.
Touble initiating solid food swallow.
Tx: surgery
STOMACH

DYSPEPSIA
Recurrent upper abdominal pain or discomfort
If < 45yo and no red flags H.pylori test if positive treat, if no response EGD
If age >45yo or anemia or weight loss or dysphagia do EGD
If dyspepsia 2 to NSAIDs stop NSAIDS and start PPI
H. Pylori Tx: amoxi, clarithro and omeprazole. Confirmation of treatment 4 weeks after completion of therapy.
Stool ag if pt continues on PPI
After eradication of H pylori may lead to reflux symptoms due to increase acid production.
Recurrent upper abdominal pain or discomfort
If < 45yo and no red flags H.pylori test if positive treat, if no response EGD
If age >45yo or anemia or weight loss or dysphagia do EGD
If dyspepsia 2 to NSAIDs stop NSAIDS and start PPI
H. Pylori Tx: amoxi, clarithro and omeprazole. Confirmation of treatment 4 weeks after completion of therapy.
Stool ag if pt continues on PPI
After eradication of H pylori may lead to reflux symptoms due to increase acid production.

PEPTIC ULCER DISEASE
If severe abdominal pain and recent use of NSAIDs and corticosteroids, think of perforated PUD, do abdominal films before EGD.
EGD if alarm symptoms.
In GI bleeding, first stabilize pt then EGD
Increase risk of rebleed: Visible vessel in EGD 50% or adherent clot in EGD 30%
If EGD shows clean base ulcer and pt stable you can send pt home same day.
If endoscopic treatment failed to control bleeding do surgery.
When IV PPI? 72h after EGD and endoscopic treatment.
If severe abdominal pain and recent use of NSAIDs and corticosteroids, think of perforated PUD, do abdominal films before EGD.
EGD if alarm symptoms.
In GI bleeding, first stabilize pt then EGD
Increase risk of rebleed: Visible vessel in EGD 50% or adherent clot in EGD 30%
If EGD shows clean base ulcer and pt stable you can send pt home same day.
If endoscopic treatment failed to control bleeding do surgery.
When IV PPI? 72h after EGD and endoscopic treatment.
GI BLEEDING
- PUD
- Mallory Weiss tears
- Esophageal varices
- Aorto enteric fistula (if h/o AAA repair and presents with melena) do EGD and CT
- Osler Weber Rendu: telagentasia, h/o nose bleeding, family history
- Peutz Jeghers Sd: hyperpigmentation of mucosas, hamartomas of GI tract
- PUD
- Mallory Weiss tears
- Esophageal varices
- Aorto enteric fistula (if h/o AAA repair and presents with melena) do EGD and CT
- Osler Weber Rendu: telagentasia, h/o nose bleeding, family history
- Peutz Jeghers Sd: hyperpigmentation of mucosas, hamartomas of GI tract

ZOLLINGER ELLISON SYNDROME OR GASTRINOMA
Chronic diarrhea with bad esophagitis or PUD.
Ulcer disease: gastric , duodenal, esophageal
Elevated serum gastrin
w/u: somatostatin receptor scintigraphy, EUS
If you cant find it do surgical exploration
Chronic diarrhea with bad esophagitis or PUD.
Ulcer disease: gastric , duodenal, esophageal
Elevated serum gastrin
w/u: somatostatin receptor scintigraphy, EUS
If you cant find it do surgical exploration

CARCINOID
GASTRIC CANCER
1) Adenocarcinoma
More in esophagus gastric junction.
2) Lymphoma: diffuse histiocitic lymphoma (better prognosis than adenocarcinoma)
* MALT: treat H.pylori and follow with EGD after months
1) Adenocarcinoma
More in esophagus gastric junction.
2) Lymphoma: diffuse histiocitic lymphoma (better prognosis than adenocarcinoma)
* MALT: treat H.pylori and follow with EGD after months
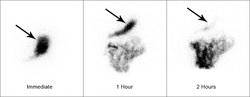
GASTROPARESIS
Nausea, abdominal pain, satiety, fullness
Nuclear medicine gastric emptying scan and EGD (to r/o other causes)
Anticholinergics, DM (usually type 1), scleroderma, post vagotomy and idiopathic.
Tx: Metoclopramide 10mg before meals (only pro motility agent), stomach pacemaker
Example: DM type 1 uncontrolled with satiety and fullness
Nausea, abdominal pain, satiety, fullness
Nuclear medicine gastric emptying scan and EGD (to r/o other causes)
Anticholinergics, DM (usually type 1), scleroderma, post vagotomy and idiopathic.
Tx: Metoclopramide 10mg before meals (only pro motility agent), stomach pacemaker
Example: DM type 1 uncontrolled with satiety and fullness
bowel

CROHN DISEASE
Onset: 20s
Family history on 20%
Pain and no bloody diarrhea
Peri rectal fistula or abscess.
Associated with smoking
Dx: colonoscopy (patchy or skip lesions, bp shows granulomas, chronic inflammation)
String sign on crohn ileitis
Complications:
* Calcium oxalate kidney stones
* Pigment Gallstones
* Vitamin B12 deficiency, vit D malabsorpsion, Hypocalcemia
*Bile induced diarrhea (<100cm resected/ cholestyramine)
* Steatorrhea >100cm resection treat with low fat diet and supplement of medium chain triglycerides
Tx:
Mild to Moderate: Mesalamine (side effect interstitial nephritis), sulfasalazine (only on colon), budesonide (ileal crohn)
Acute flare prednisone
Severe: Azathioprine (side effect bone marrow suppression) , 6MP
Fistula, severe Crohn not responding to treatment: TNF antagonist Infliximab , adalimumab or certolizumab
Perianal fistula and abscess: metronidazole (side effect neuropathy)
Increase risk for DVT
Onset: 20s
Family history on 20%
Pain and no bloody diarrhea
Peri rectal fistula or abscess.
Associated with smoking
Dx: colonoscopy (patchy or skip lesions, bp shows granulomas, chronic inflammation)
String sign on crohn ileitis
Complications:
* Calcium oxalate kidney stones
* Pigment Gallstones
* Vitamin B12 deficiency, vit D malabsorpsion, Hypocalcemia
*Bile induced diarrhea (<100cm resected/ cholestyramine)
* Steatorrhea >100cm resection treat with low fat diet and supplement of medium chain triglycerides
Tx:
Mild to Moderate: Mesalamine (side effect interstitial nephritis), sulfasalazine (only on colon), budesonide (ileal crohn)
Acute flare prednisone
Severe: Azathioprine (side effect bone marrow suppression) , 6MP
Fistula, severe Crohn not responding to treatment: TNF antagonist Infliximab , adalimumab or certolizumab
Perianal fistula and abscess: metronidazole (side effect neuropathy)
Increase risk for DVT

ULCERATIVE COLITIS
MICROSCOPIC COLITIS
Inflamation of the colon. Can be collagenous or lymphocytic
Sx Watery diarrhea
Tx: anti diarrhea meds and if it fails then Budesonide
Inflamation of the colon. Can be collagenous or lymphocytic
Sx Watery diarrhea
Tx: anti diarrhea meds and if it fails then Budesonide

MECKEL DIVERTICULUM
Most common congenital GI anomaly. 50% GI bleeding in children.
Can cause obstruction, intussusception.
Dx: Technetium scan
Most common congenital GI anomaly. 50% GI bleeding in children.
Can cause obstruction, intussusception.
Dx: Technetium scan
LOWER GI BLEEDING
- Diverticulosis (painless) most common
- Arteriovenous malformation (AVM) and angiodysplasia [ are associated with ESRD or AS (mid systolic murmur)]
- Colon cancer, polyps and s/p polypectomy
- Ischemic colitis (pain)
- Duodenal ulcer
- Meckel diverticulum (young patient)
- Hemorrhoids
- Diverticulosis (painless) most common
- Arteriovenous malformation (AVM) and angiodysplasia [ are associated with ESRD or AS (mid systolic murmur)]
- Colon cancer, polyps and s/p polypectomy
- Ischemic colitis (pain)
- Duodenal ulcer
- Meckel diverticulum (young patient)
- Hemorrhoids

HEREDITARY HEMORRHAGIC TELANGIECTASIA
(OSLER-WEBER-RENDU)
History of epistaxis
PE: telangiectasias lips and fingers
Family history of AVM, epistaxis, telangiectasia
AVM
(OSLER-WEBER-RENDU)
History of epistaxis
PE: telangiectasias lips and fingers
Family history of AVM, epistaxis, telangiectasia
AVM
CHRONIC MESENTERIC ISCHEMIA
* Triad
- Post prandial abdominal pain
- Decreased pain with smaller meals, weight loss
- Abdominal bruit
* Dx: CT angiogram first, Mesenteric angiogram
* Triad
- Post prandial abdominal pain
- Decreased pain with smaller meals, weight loss
- Abdominal bruit
* Dx: CT angiogram first, Mesenteric angiogram
INTESTINAL INFARCTION
Acute arterial embolization
In a pt with afib, valve disease or post MI
Acute abdominal pain out of proportion with physical exam
High amylase
Dx: Angiogram
Tx: Surgery
Acute arterial embolization
In a pt with afib, valve disease or post MI
Acute abdominal pain out of proportion with physical exam
High amylase
Dx: Angiogram
Tx: Surgery
PANCREAS



